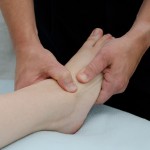
In the previous post I had hoped to serve you by discussing my general thoughts and perspective on the Anterior Thorax. This section will be a discussion on some basic assessment techniques and perspectives I regularly utilize for the anterior thorax.
When looking at treatment for the anterior thorax, the manual therapist must have a good knowledge of the anatomy of the exterior and interior thoracic cage. One book I recommend is “The Thorax” by Jean-Pierre Barral. It is a great resource and I refer to it on a regular basis.
From Amazon:
Barrral begins by describing the thorax as an area of conflict and contrast: it must protect the organs enclosed within, yet must also allow exchanges with the neck and abdomen. Problems with either of its dual roles of protection and exchange lie at the root of most thoracic disorders. Detailed descriptions and illustrations are provided of tests for dysfunction and treatment of the nonaxial joints, fasciae and viscera of this important area of the body.
Among the special topics contained in this volume are global and local listening of the thorax; utilization of the completed Adson-Wright test; cervical attachments of the pleura; intrasternal tests and treatment; utilization of various access points to the phrenic nerve; and stretching along the orientation of the coronary arteries.
I couldn’t agree more with this description.
Complaints
There are a number of patient complaints that we see every day; shortness of breath, tight exterior chest and or back, sharp specific and or shooting pain, deep pain, referred pain/tension, the inability to breathe deeply etc… There are also complaints from condition such as asthma, post surgical trauma, post unforeseen trauma such as MVA, strains, sprains, fractures, contusions etc…
As with all patients complaining of dysfunction in the thorax, a detailed thorough history must be done to rule out conditions that are outside our scope of practice and may require immediate emergent care. I have had a few times in my practice where I’ve caught a Myocardial Infarction and called 911. If this has yet to happen to you, be forewarned, it will.
A future article will deal with information gathering during history taking.
Orthopaedic Tests
So, the question is how do we assess and come to a treatment plan for a patient in discomfort? There are a number of assessment tests that are available to utilize. There in lies the problem. There is much research that shows that these tests are unreliable due to user perception, testers reliability and testers education on the application of the tests. Therapists perform the same tests on the same patients and come to completely different conclusions. This happens more often that we would all like to believe.
So do we throw out all the tests, books written on the tests and our education? Well… not yet! My suggestion to you is to have a few books written on orthopaedic testing in your library. Refer to each of them on a regular basis and compare/contrast the application of the tests. Once you have become familiar with them, choose 3/body part that you feel you are capable of performing. These should be committed to memory and should be practiced on a regular basis. Make these part of your regular routine diagnostic assessment portion of your treatments. Your goal is to become very skilled in the investigative art of attempting to understand what possibly is causing your patients complaint.
In my office I created orthopaedic assessment paper that had a list of my commonly used tests and expected positive and negative outcomes for each region of the body. I did this to make it easier to remember the tests and before long, this list was imprinted in my mind through my eyes.
Remember that we don’t just perform tests willy nilly. There has to be an underlying reason. The patient must have some complaint that leads you to testing. Pain, tension, loss of AROM/PROM, headache, referred pain/tension and so on must be investigated. Initially attempting to investigate the complaint with orthopaedic testing is the logical starting point.
One main problem I find is that there are too few orthopaedic tests for the thoracic cage. There are Specific AROM tests for vertebralcostal joints, Sternochondral joints, and you can usually feel for a decreased intercostals space and there are tests for extremity’s with neurological/vascular complaints, loss of AROM etc… but what about torsional strain feelings behind the sternum? What of pain over the heart where the heart has been ruled out? What of pain within the chest sometimes described as being in between? What of respiratory challenges? Sure there are medical tests that can confirm what the patient is complaining of, but why? In cases such as these and many more, you must rely on your sensing/palpatory abilities and patient observational skills to make the determination of what a possible cause may be.
How to acquire information
In my previous post “The Thorax Part 1”, I very briefly suggested that you commit yourself to not palpate, but to “sense” for information your patients body is attempting to relay to you. I find these listening skills come into place more and more with concerns of the thorax.
Develop your “allknowingseeingthinkingfeeling” hands.
I utilize a combination of palpatory and sensing techniques together. Try the following:
standing above your supine patient at their head, placing your full palm onto their sternum. Slowly and firmly load down into the table  and inferiorly through the sternum. What to you feel? Does the tissues take you straight, or is there something that takes you into either a rotational or diagonal direction or a combination of both? Come back out and this time perform the same action with less force of compression. Do this over and over until you get to the point where you can feel the direction of ease of the tissue using the minimalist amount of compression …ounces. You are now on your way to sensing! This is a great technique for any body part.
and inferiorly through the sternum. What to you feel? Does the tissues take you straight, or is there something that takes you into either a rotational or diagonal direction or a combination of both? Come back out and this time perform the same action with less force of compression. Do this over and over until you get to the point where you can feel the direction of ease of the tissue using the minimalist amount of compression …ounces. You are now on your way to sensing! This is a great technique for any body part.
“Co-operate with the tissues, you’ll get more with less!”
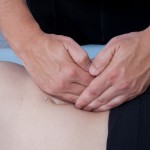
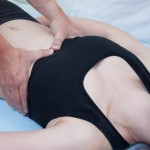
Now move to one side of the table. Working cross body, place both of your hands onto the chest wall, one placed on the upper ribs 1-4, 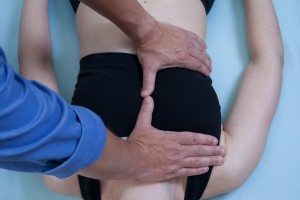 and one place on the lower ribs 6-10. If you patient is female, the breast tissue will be in between your hands, but our focus is still the thoracic tissues. Perform this exercise once again. Does the tissue take one hand in a different direction than the other? Does the whole cage move easily down into the table or is there some kind of diagonal/rotational torque. Do the upper tissues move differently than the lower tissues?
and one place on the lower ribs 6-10. If you patient is female, the breast tissue will be in between your hands, but our focus is still the thoracic tissues. Perform this exercise once again. Does the tissue take one hand in a different direction than the other? Does the whole cage move easily down into the table or is there some kind of diagonal/rotational torque. Do the upper tissues move differently than the lower tissues?
Information acquired can change with small movements of the head, neck & arms. Don’t be afraid to move your patient or have them move. Load into the sternum once again with either of the techniques described above and have the patient rotate their head one direction then the other. Look for subtle changes not only in what you can sense, but also in feedback from the patient.
What are you feeling; Skin, Superficial fascia, muscle, deep fascia, bone, ligament, joint capsule, endothoracic fascia, parietal/visceral pleura, lung, mediastinum, neurovasculature, pericardium, oesophagus, trachea, vertebral rotations, fluid dynamics, tissues of the same side or opposite side? I find it’s always a good idea to have a Netter Anatomy around when trying to be specific as to what tissues are speaking to me.
Don’t forget to monitor to your patients heart rate and thoracic respiration. These are great systems that let you know when you are close to the source of a patient’s complaint(s).
“The quieter the mind, the stiller the hands, the less movement we make, the more we are able to perceive involuntary movement.”
– James Jealous, DO
Look for health!
Where is the health, where is the restriction? We all seem to be very focused on finding the restrictions, tension, pain, but how often do you look for the health in the tissue? How often do you look for what is working pain free? Look for the health in every patient at some point. It’s quite refreshing to watch the physiology work as a well sounding orchestra! Music not only to your hands, but to your physiology also. Time seems to stop in this place… enjoy it.
Conclusion
As always, I hope that I have been able to serve you in some way with this information, be it a completely new perspective into your patients, be it some new thoughts about how to approach a treatment or provide you with a review and acknowledgement that what you are doing, as far as I’m concerned, is having an amazingly positive impact in improving the quality of life for your patients.
For information on our Thorax, Abdomen & Pelvic course see the Course Description.